
Dave deBronkart, known as e-Patient Dave, is a thought leader and pioneer in patient empowerment, e-patient advocate and chief patient officer at PocketHealth
Before the Internet, health care organizations served as the primary source of information and knowledge regarding medical care. But once people had access to more information and formed robust social communities and connections on the web, a new generation of e-patients came to life – like COVID-19 long haulers.
In a recent #MayoSHSMD keynote presentation, Dave deBronkart, known as e-Patient Dave, a thought leader and pioneer in patient empowerment, e-patient advocate and chief patient officer at PocketHealth, recently described how social media enabled long COVID-19 patients to define their condition and attract the attention of the medical community.
“Dr. Warner Slack, an informatics pioneer in the 1970s, once said, ‘Patients are the most under-used resource in health care,’” said deBronkart. “There is more to an ideal outcome than what’s in the textbook… Things are very different from how they were one or two decades ago. For health care to achieve its true potential, the best available information has to be at the point of need.”
COVID-19 patients who weren’t getting better found each other online through Google or social networks like Facebook.
“Medicine didn’t know what to make of their reported symptoms, and so they banded together to characterize what the disease was like,” said deBronkart. “This is excruciatingly important to realize. Traditionally when there is a bunch of symptoms, scientists and physicians were the ones who would have characterized a disease. This time, nobody had time for that and the patients did that themselves.”
The voices of COVID-19 long haulers were heard and attracted so much media attention that the National Institutes of Health (NIH) announced May 20 they would research long term symptoms of the virus.
The Active e-Patient
One important detail, stressed by deBronkart, is that “patients playing an active role in their health care doesn’t mean they don’t feel they need providers.” He, especially, knows the truth of this. deBronkart sought connections on the Internet 14 years ago in an effort to save his life after being diagnosed with stage four kidney cancer.
“A pivotal moment… is that my doctor prescribed ACOR.org, a cancer patient listserv, now smartpatients.com,” said deBronkart.
Within two hours of joining, he connected with other kidney cancer patients who informed him of a potential treatment, high-dose IL-2 (HDIL-2), an immunotherapy, which was associated with severe side effects, but sometimes worked. His peers also shared four oncologists in his area that used HDIL-2.
“I wasn’t trying to be the doctor, I was trying to be as involved as I could,” said deBronkart.
He proved to be one of the lucky ones who respond to HDIL-2. Almost immediately, his tumors started to shrink and his treatment ended in less than four months. He gave speeches sharing his story, which eventually caught the attention of the British Medical Journal (BMJ), who requested he share it with their readers. In 2013, BMJ.com published, “How the e-patient community helped save my life: an essay by Dave deBronkart.” In his essay, he describes how being an informed patient helped direct his treatment plan.
In this new era of the e-patient, sometimes the most useful and relevant up-to-the-minute information can exist outside of traditional channels. deBronkart explains how the shift from a closed system to an open network has enabled a greater transfer of information. In what he refers to as “health care 2.0,” [organizations] and individuals were able to connect, and in “health care 3.0,” everyone becomes interconnected to form “information capillaries,” a broad network of groups that share an enhanced level of information.
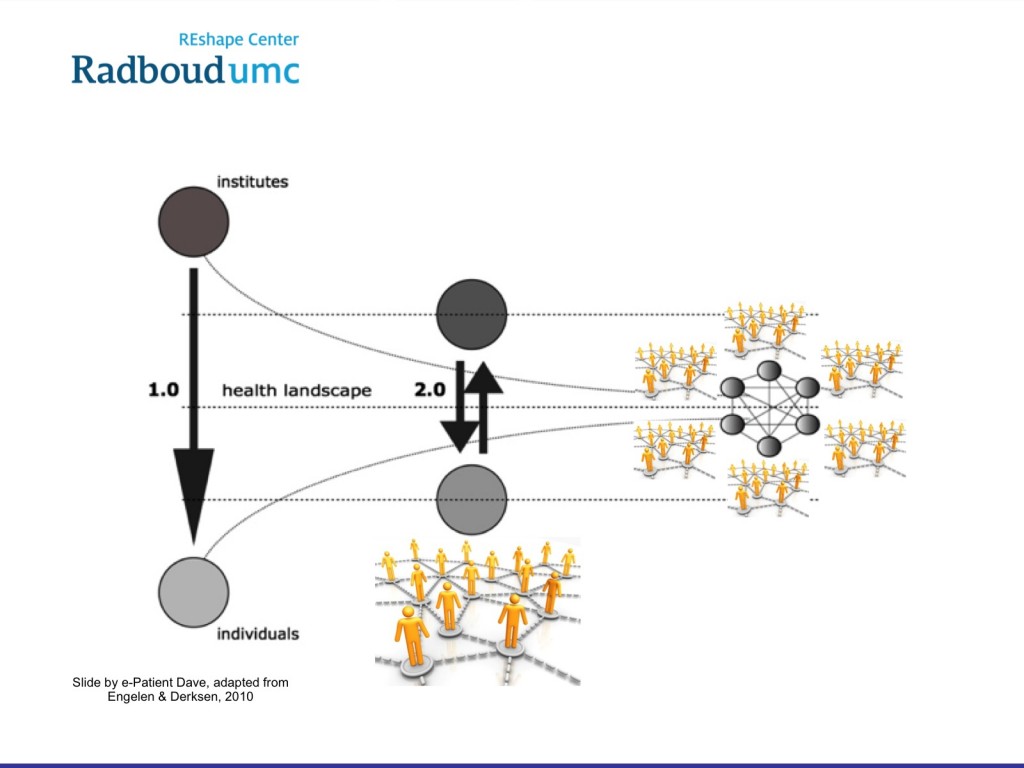
The diagram above was published by Dutch guru Lucien Engelen, who in the same year decided to
create a TED conference where nearly half of the speakers were actual patients, including Dave deBronkart.
He went on to becomeone of LinkedIn’s first influencers, and is today part of Deloitte’s Center for the Edge.
He shared a diagram adapted from Lucien Engelen illustrating how communication networks have changed over time. “This diagram was visionary when it was created in 2010 – a lifetime ago in social media years,” said deBronkart. “Yet it doesn’t just apply to doctor-patient relationships. Look – it precisely illustrates the change we must acknowledge in hospital marketing. A decade ago it was all one-way push, but then patients started learning from each other too.”
Health care 3.0 includes robust and complex social networks. “Today, on the right, it’s easy to see that one-way doesn’t cut it anymore. To have influence, marketers first need to listen to what’s in the conversational stream, or our contributions will be drowned out. Then we need to add messaging that can be heard by, and will make sense to, that vast external network of conversations, because it’s going on with or without us… and if we don’t hear what they’re saying, then just as the long COVID-19 patients did, they’ll ignore us and take matters into their own hands.”
He quotes Susannah Fox, a former researcher at Pew Research, “Peer health communities can fill in gaps left by traditional care teams.” With enormous pressures in health care, patients working together with clinicians can bridge opportunities of care.
Listening and Adapting
deBronkart emphasizes that health care marketers, communicators and strategists need to be prepared for the unexpected as the health care landscape changes rapidly. He suggests:
- Listen to what it’s like to try and get care when your hospital is overwhelmed.
- Listen to how patients have been banding together without help and gathering and analyzing data.
- Listen to what they’ve learned – like how COVID-19 long haulers joined together to collect data through their own surveys, discovering important findings six months before academia caught up.
He also recommends the following books that align with themes of today’s e-patient:
- The Half-Life of Facts by Samuel Arbesman explores how it takes time for information to travel. It notes how the half-life by which knowledge becomes obsolete is greater in health care than in any other field.
- Thinking, Fast and Slow by Nobel-prize winning Daniel Kahneman uncovers how technology is developing very rapidly, possibly exponentially, but people have a difficult time adapting because they tend to think in a linear fashion. This thinking could be applied to reason why populations were not equipped to grasp the spread of a virus like COVID-19.
As seen with long COVID-19, remaining flexible and vigilant on social media and other digital channels will give patients the opportunity to make contributions to the complexities of medicine. In the sign off of his BMJ.com essay, deBronkart calls for health care professionals to listen to patents and adapt to their needs.
“Please, let patients help improve health care. Let patients help steer our decisions, strategic and practical. Let patients help define what value in medicine is.”
Learning More